Download Medieval Medicine Worksheets
Do you want to save dozens of hours in time? Get your evenings and weekends back? Be able to teach Medieval Medicine to your students?
Our worksheet bundle includes a fact file and printable worksheets and student activities. Perfect for both the classroom and homeschooling!
Table of Contents
Add a header to begin generating the table of contents
Summary
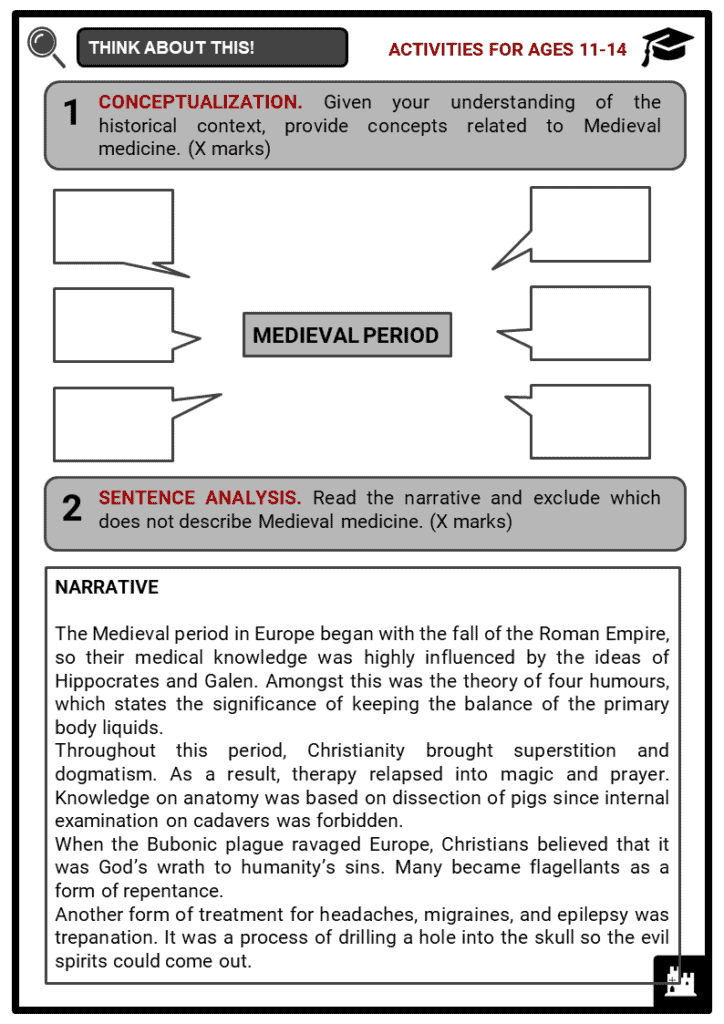
- Brief historical background during the Medieval Period.
- Features of Medieval medicine, including diseases, cures, and beliefs.
- The Black Death and how medieval people reacted to it.
- Health risk of people during the Middle Ages.
Key Facts And Information
Let’s know more about medicine during the Medieval Period!
- Medical knowledge during the Middle Ages was derived from the Greco-Roman. In general, medieval civilisations carried out medical practices that today are considered unhygienic, hazardous, and unreasonable. Therapy relapsed into magic and prayer, fantastical and often revolting concoctions, charms and amulets, and faith healing.
- The superstition and dogmatism that marked the rise of Christianity in Europe continued to flourish throughout the Middle Ages. Free inquiry, observation, experiments were out of the question; learning, including magical learning, was devoted to the study of the ancient authoritative texts.
- Historically, the Middle Ages occurred after the fall of the Roman Empire and lasted until the English Reformation. The period is characterised by feudalism and high reliance on knowledge from the Church.
Features of Medieval medicine
- Run by feudal lords, small territories in the Middle Ages were populated by rural servitude. There were no public health services and communication was poorly utilized.
- As a result, many believed in superstitions. They could not read or write. Monks were the only people who were educated and had the chance to teach philosophy and science.
- When the Roman Catholic Church dominated the era, spells replaced prayers to saints. Moreover, people began to practice penance and pilgrimages for repentance for sins.
- With the emergence of monks as healers, monasteries became the home of the sick and dying.
- Venesection and various herbs were used widely. Dissection of cadavers was completely forbidden, and anatomy, if studied outside of textbooks, was based on the dissection of pigs.
- Hygiene and sanitation were at a very low level since the human body was held in contempt.
- The demonic theory of disease again gained ascendancy, or else, as in the case of the devastating plague epidemics, the blame was placed on the Jews.
- Throughout the Middle Ages, only the wealthiest could afford physicians. On the other hand, the poor were obliged to consult local practitioners that referred to folkloric traditions.
- Medieval cures
- Historians suggest that in addition to herbal medicine, medieval people used several treatments in attempts to cure diseases. It includes:
- Application of leeches
- Bleeding
- Smelling of strong posies
- Cutting and draining of buboes
- Trepanning
- Praying and whipping
- Moreover, surgeons at that time also attempted internal surgical procedures to heal wounds, set broken bones, cure eye cataracts, and extract bladder stones. However, the mortality rate was high due to pain, infection and bleeding.
- Historians suggest that in addition to herbal medicine, medieval people used several treatments in attempts to cure diseases. It includes:
Take a closer look!
- Trepanning was a surgical procedure in which a hole is drilled into the skull to treat intracranial ailments. The screw-like saw and holder were believed to treat seizure and mental disorders.
- Based on archaeological finds, trepanning or trephination was already a medical practice since the Neolithic period. Many ancient cultures believed that by drilling a hole in the skull could cure a person’s disease by casting off the evil spirit.
Life expectancy in Medieval Europe
- During this period, sudden and premature death was common, especially among the peasantry. Those who survived adulthood usually died from diseases, warfare and famine. For women, childbirth was a common cause of death. For example, Jane Seymour, King Henry VIII’s third wife died of giving birth to future Edward VI in 1537.
Theories of medicine
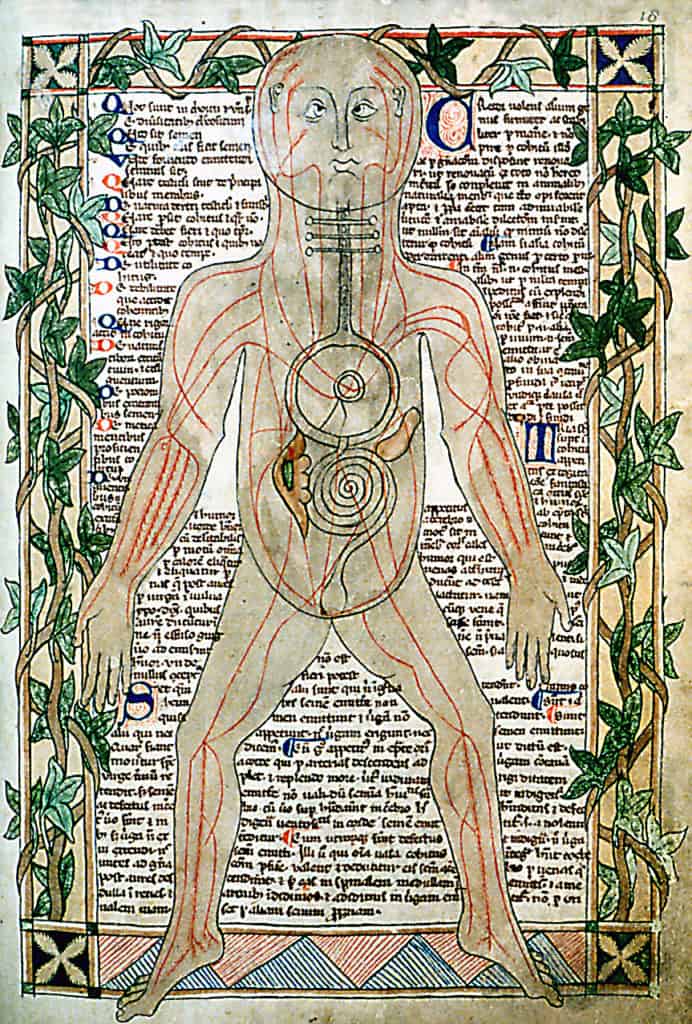
- Influenced by the works of Hippocrates and Galen, Medieval people primarily based their understanding of the human body based on the theory of four humours. It states that four principal fluids in the body need to be in balance.
- Through herbal medicine, diet and bloodletting (using leeches) the balance of the humours could be achieved. It is believed that the theory of four humours was based on astrological signs of the zodiac. Below is the theory of four humours in the table.
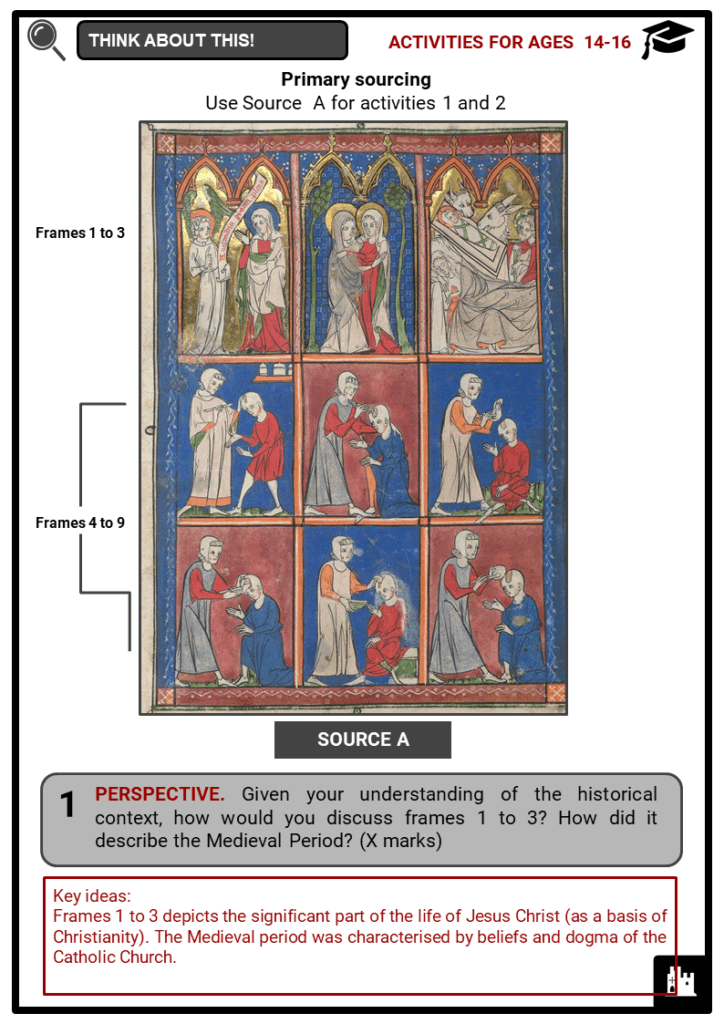
- The most common medieval belief in the existence of diseases was rooted in Christianity. The church thought illness was a form of punishment from God, and order to recover, the person must repent from sins.
- Since diseases were considered as God-sent, Christians were the only people who could cure. An example were monks, known as divine physicians. They used prayers and other liturgical practices to treat diseases.
- Although herbalism was an ancient remedy to cure diseases, by the 16th century it became a rapidly developing discipline. In addition to monasteries, universities also set up gardens for students to examine plants.
Medieval hospitals
- Monasteries were run by nuns and monks who believed it was their Christian duty to care for the sick.
- As such, health and religion were closely connected.
- Wealthy Christians financed monasteries, which had plumbing, toilets, and clean water.
- However, these hospitals refused to admit lepers, lunatics, and people with falling sickness or contagious diseases.
- No pregnant women or women with breastfeeding infants. No intolerable people even if they’re poor or infirm. If anyone of these were admitted by mistake, they’re to be expelled immediately.
- Things only really began to change in the 18th century when new hospitals were built with wards for different diseases.
The School of Salerno
- The famous School of Salerno which flourished from the X to the XIII century was the first organised medical school in Europe. It was probably also the most enlightened. The Greek, Latin, Arabic, and Hebrew influences merged in Salerno, and it was known as the Hippocratic City. The curriculum required three years of preliminary studies and five of medical; the graduate received the degree of Magister of Doctor, and the practice of calling a physician a ‘Doctor’ derives from Salerno.
- According to laws promulgated in 1240 by Emperor Frederick II, a year of postgraduate practice under an established physician was required before the graduate was licensed: ownership of an apothecary shop, or any business relation with an apothecary, was forbidden, and preparation of drugs was supervised by inspectors.
- The School of Salerno had many famous graduates. Its Regimen Sanitatis, a compendium of domestic medicine in the form of proverbs, was among the most popular books of the Middle Ages.
- Women were admitted to the School, but it is not certain whether as nurses, midwives or physicians. For all its comparatively advanced character, Salerno still regarded suppuration as part of the natural wound healing, and its first textbook on anatomy was based on that of the pig.
- The connection of Constantinus Africanus (1010-1087) with the School of Salerno is uncertain, though he is known to have spent some time there and at the Benedictine monastery of Monte Cassino.
- Constantinus is known best for his extensive translations from the Arabic into Latin; in this way, he brought back to the West its lost Greco-Greco-Roman heritage.
- Subsequently, Avicenna, Haly Abbas, and Maimonides, as well as Galen and Hippocrates, became entrenched in all the schools of Medieval Europe.
- After the decline of Salerno, at the end of the XIII century, the medical schools of Montpellier, Bologna, Padua, and Paris came into prominence, but their contribution to medical evolution was slight.
The Black Death: Medieval epidemic
- When the bubonic plague started in Europe due to the widespread unhygienic habits, people were not aware that the main cause of death was the bacteria Yersinia pestis, which was spread by infected rat’s fleas. Not having a scientific explanation for the disease that had wiped out over one-third of Europe’s population, people attempted to save their lives in a variety of ways.
- Manifestation of the disease
- When the plague started manifesting in a person’s body, it would initially appear as common flu with chills and feelings of weakness.
- In the next 24 hours, the bacteria spread across the lymphatic system before affecting the skin and internal organs.
- Subsequently, it caused ‘severe trembling accompanied by profuse sweating, subcutaneous haemorrhaging, and painful, dark reddish-purple spots rapidly developed.
- In addition, painful hypersensitive buboes formed in the lymph nodes of the armpit and groin. The buboes swelled as large as oranges and filled up with pus and blood.
- If the buboes were not carefully lanced, the infection caused blood poisoning, and further spreading of the disease happened when the buboes burst (Bardot 2019).
- Reaction to the disease
- In an age when religion ruled society and its thought, it is not surprising that the black death was considered a divine punishment inflicted by God to sinful members of humanity. In fact, some Christians who believed such theory punished themselves severely through self-flagellation.
- Others thought that the best solution to avoid the plague was hiding in the sewers, where no one could reach them, see them, or touch them. However, the filthy conditions of the sewers, with their foul-smelling surroundings and fetid insects, did not save them from death, and although they may not have been infected by the bubonic plague, they nonetheless died due to other sever illnesses and infections.
- Other practices involved drinking arsenic or mercury, not having thoughts about death in general, not having thoughts about the plague, not having sad thoughts, not eating figs, not eating meat, not running or walking outside, not exercising at all, not bathing, not sleeping in the day, and finally for good measure, not having sex’ (Sheriff 2013).
- Richer people, on the other hand, ingested a crunchy mixture of crushed emeralds and powdered stones either with a drink, or with food such as bread.
- Aromatherapy was also employed, and individuals were encouraged to carry flowers with a sweet scent or herbs.
- Cutting open the buboes filled with pus and blood, and applying a thick layer of human excrements, resins, and flower roots.
Dangers during the Medieval period
- Some historians suggest that the Medieval period was among the most turbulent yet transformative era in European history. Here is the list of risks faced by medieval people related to health and medicine.
- During the 14th and 15th century, the Black Death, also known as the Bubonic plague was the greatest killer that diminished almost half of Europe’s population.
- By the late 14th century, life expectancy in Italy became under 20 years old. A large number of casualties were children, who were most vulnerable to the disease. Other epidemics, such as tuberculosis, smallpox, dysentery, typhoid, influenza, and mumps were also deadly.
- Due to bad weather conditions and poor harvests, famine and malnutrition became a serious problem during this period. Many suffered from diseases, while others starved to death. In the early 14th century, the Great Famine was caused by incredibly heavy rainfall.
- During the Medieval period, giving birth was a perilous event for women. Labour period was fatal to both mother and child. Most midwives had no formal training. Women were prone to die of exhaustion during labour, while others who survived it could still die of postnatal infections.
Image sources:
[1.] https://upload.wikimedia.org/wikipedia/commons/1/12/13th_century_anatomical_illustration_-_sharp.jpg
[2.] https://upload.wikimedia.org/wikipedia/commons/a/a4/ScuolaMedicaMiniatura.jpg
[3.] https://upload.wikimedia.org/wikipedia/commons/1/1e/Great_plague_of_london-1665.jpg